Introduction
Knee osteoarthritis (KOA) is a chronic slowly progressive and debilitating condition, which is characterized by pain, limitation of physical activity. It is a leading cause of disability, impaired quality of life and activities of daily living [1].
Traditionally, knee osteoarthritis is considered as a degenerative disease because of cartilage degeneration, loss of joint space and osteophyte formation in radiography, but recent observations indicate existence of an inflammatory process which involves the whole tissues of the joint, and contributes to the development of symptoms and progression of structural changes [2, 3].
Mechanical and biochemical factors are also responsible for the development of synovitis, cartilage breakdown, osteophytes formation, subchondral bone sclerosis and alterations in the joint capsule [3]. Synovial membrane inflammation is important, because it is linked with symptoms such as joint pain, effusion, joint dysfunction, and progression of structural changes and cytokines abnormalities [4–7].
Reduction of osteoarthritic pain by anti-inflammatory drugs supports an association between inflammatory process and pain. However, response to anti-inflammatory drugs in KOA is complex. It is partly dependent on the patterns of clinical symptoms, type of involved joints and responsible factors of pain [8, 9]. Existing data suggest that targeting synovial inflammation at early stage of KOA may provide a possible beneficial effect in delaying cartilage damage or osteophytes formation [4, 5, 10].
Several treatment guidelines have been established to relieve pain, improve function and prevent clinical exacerbation in knee osteoarthritis [11]. Multiple medications including systemic and local non-steroidal anti-inflammatory drugs (NSAIDs), acetaminophen, opioids which have been considered for treatment of KOA are effective only in a proportion of patients.
In non-responders to standard therapy, particularly in patients with joint effusion, many drugs are administrated through intra-articular injection to attain a rapid benefit through direct effect on synovial inflammation [11, 12].
About 50% of patients with KOA have synovitis and joint effusion at the time of arthroscopy. Severity of synovitis correlates positively with pain, and shrinkage of synovial tissue volume correlates with treatment response [13, 14]. Hence, suppression of synovial inflammation has been considered as the main target of treatment for pain relief [10].
Unlike most osteoarthritis drugs, intra-articular corticosteroids (IACS) are safe, inexpensive and well tolerated by patients. Because of their moderate analgesic effect, they can be considered for pain relief in patients who are not responsive to conventional medications [15].
The beneficial effect of intra-articular corticosteroid in KOA is assumed to be mediated through its anti-inflammatory effect against synovial inflammation which is an integral part of osteoarthritis (OA) process. However, efficacy of intra-articular corticosteroids in KOA depends upon the presence, extent and severity of synovitis and its association with pain [14, 16]. However, the prevalence of synovitis varies across different study populations and is dependent to its definition and diagnostic methods [17, 18].
At present, it is not possible to determine which patients gain the most therapeutic benefits from IACS treatment. Based on anti-inflammatory characteristics of IACS, it is hypothesized that, patients with knee joint synovitis and effusion, or KOA patients with clinical exacerbations will attain greater benefit from IACS therapy.
In particular, individuals with minimal cartilage destruction are expected to attain most improvement in knee function [10, 11]. However, the results of many meta-analyses and RCTs which addressed efficacy of IACS in KOA are conflicting, and the outcomes of treatment vary from no efficacy or little short duration of improvement in pain and/or joint function to a few or several weeks of pain relief [14, 16, 19–21].
Inconsistent results can be attributed to variations in study design, outcome measures, patients selection, treatment strategy, duration of follow-up period. Other factors such as presence or absence of synovitis, joint effusion, severity of structural lesions, severity of synovial inflammation, sources of pain, accuracy of intra-articular injection can also affect treatment responses [8, 22].
Even intra-articular injection of normal saline, or joint fluid aspiration itself can provide pain relief [7, 16]. A meta-analysis of 32 studies involving 1705 patients revealed a significant long-term pain reduction by intra-articular injection of normal saline in patients with knee osteoarthritis [23].
Yet, it is difficult to predict the therapeutic effect of IACS, and to discriminate patients who are responders or non-responders. Hence this narrative review aims to elucidate the effect of IACS in KOA and to recognize the factors that predict treatment response by review of the existing data. Treatment response was defined as pain relief or significant pain reduction with or without functional improvement for one week or longer duration after IACS therapy or prevention of structural progression in long-term studies.
For these purposes, English language databases were searched as recommended to identify potential studies which have been published in Medline/PubMed, Scopus and Google Scholar since 2000 by using keywords such as knee osteoarthritis, synovitis, effusion, intra-articular corticosteroid, efficacy, treatment, pain relief, functional improvement, predictors. In addition the references of the selected papers were searched to find eligible studies.
Studies in which pain relief with or without functional improvement or changes in pain was considered as an outcome and was evaluated by either Visual Analogue Scale (VAS) or Western Ontario and McMaster Universities OA Index (WOMAC), or other valid measures were selected. Studies without pain assessment were excluded.
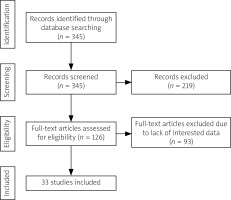
A total of 345 studies were found which 219 papers were irrelevant based on the titles and so were excluded. Among 126 remaining full-text 93 studies were not eligible due to lack of interested data and removed. A total of 33 full-texts which have been found to be interest were selected for analysis (Fig. 1).
All relevant sources were critically analyzed to ensure diversity in the sources and to avoid bias [24]. The selected studies were categorized according to study designs and the results were presented under subheadings in relation to the diagnosis and prevalence of synovitis, synovitis and pain, efficacy of IACS and predictors of treatment response.
Diagnosis of synovitis
The diagnosis of knee synovitis is important for identification of patients who are likely to benefit from IACS therapy. Fluctuations in synovial inflammation and joint effusion can be a sign of KOA flare or treatment response. Arthrocentesis is the best method for the diagnosis and quantification of joint effusion, but this measure is invasive and painful. Accurate estimation of total effusion by joint aspiration is often impossible [25].
A clinical diagnosis of synovitis is suspected in the presence of a swollen joint with effusion, redness, warmness, and pain. However, clinical detection of synovitis at early stage of KOA is difficult because of low specificity as well as low intraobserver and interobserver reliability of clinical examination [26].
Existence and extent of synovial inflammation can be also confirmed by ultrasonography and MRI, even in subjects with few symptoms or without clinical synovitis who have limited cartilage or subchondral bone lesions.
Moreover, synovitis can be detected as changes in thickening of synovium or localized proliferative changes by arthroscopic examination of the knee joint [4].
Prevalence of synovitis in knee osteoarthritis
Synovial abnormalities have been shown in different stages of osteoarthritis and existing data indicate an important role for synovial abnormalities in the pathogenesis of osteoarthritis [27].
About 50% of patients with KOA have synovial inflammatory changes such as thickening of synovium or localized proliferative changes [4]. Application of sensitive imaging technics and tissue examination indicated a high prevalence of synovial inflammation in all stage of osteoarthritis [1].
Nonetheless, the prevalence of synovitis in KOA varies across different studies according to diagnostic measures. In one large study of patients with symptomatic KOA, 46% of patients had synovial inflammation or joint effusion on sonographic examination [17]. By using contrast-enhanced as well as non-enhance magnetic resonance imaging (MRI), synovitis was detected in 70% of patients without joint effusion and in more than 95% of patients with knee joint effusion [18].
A meta-analysis of 24 observational studies revealed a pooled prevalence of ultrasound detected synovial effusion, synovial hypertrophy, and Doppler signal in 51.5%, 41.5%, and 23.5% of people with KOA and pain respectively [28].
Association between synovitis and pain in knee osteoarthritis
In patients with KOA several parameters including synovitis, joint effusion, meniscal tears and bone marrow lesions are associated with pain [29].
Wang et al. [27] found an independent association between MRI-detected synovitis and pain in a large cross-sectional and longitudinal study of patients with knee osteoarthritis [30].
Another longitudinal study found a relationship between fluctuations of synovitis and change in pain and cartilage volume in knee osteoarthritis. In this study changes in pain and synovial inflammation were assessed by VAS and MRI at baseline, 15 months and 30 months later. The strongest correlation was observed between pain and infrapatellar synovitis [31].
In one study, 80% of patients with moderate pain had synovitis, and there was a strong correlation between severity of pain and synovitis detected with dynamic contrast-enhanced MRI (DCE-MR). In patients with synovitis pain was 9.2 times greater than those without synovitis [32]. However, knee pain can occur in the absence of synovitis or effusion due to bone marrow lesions or intra-articular pathology [33].
Efficacy of intra-articular corticosteroids in knee osteoarthritis
Effect on knee pain and function
Most studies including RCTs, systematic review and uncontrolled clinical trials which have addressed the effect of IACS in symptomatic KOA (Table I and II) found a beneficial effect of treatment on pain, joint function, walking time as well as in range of joint motion [14, 16, 34–46]. However, these studies differ in regard to treatment outcomes and outcome measures, duration of studies and the number of IACS injections.
Table I
The results of randomized controlled trials and meta-analyses on the effect of intra-articular corticosteroids in knee osteoarthritis
| Authors (year) | Characteristics of patients, study type | Aims of studies | Results |
|---|---|---|---|
| Gaffney et al. (1995) [16] | RCT, of 84 patients with clinical and radiographic evidence of KOA | To assess the effect of IATH on pain (VAS) function (HAQ), walking time vs. placebo | Overall improvement observed in 75% of IATH vs. 49% of placebo. Significant VAS and walking time improvement at week 1 in IATH especially in patients with effusion. HAQ improved at week 1 and 6 in IATH group |
| Jones et al. (1996) [14] | RCT in 59 patients with symptomatic KOA | To determine the effect of IAMP on pain (VAS) vs. placebo | Significant reduction in VAS score after 3 weeks compared with placebo and baseline |
| Raynauld et al. (2003) [36] | A 2-year RCT of 68 patients with symptomatic KOA | To determine long-term safety of every 3 months injection of IATH vs. placebo on WOMAC pain score, night pain, range of motion and joint space narrowing | No difference in joint space narrowing at 1-year and 2-year follow-up. After 1 year there was a trend toward improvement of WOMAC pain, night pain and range of motion in IATH group vs placebo. Pain and stiffness improved significantly throughout the 2-year study |
| Chao et al. (2010) [34] | RCT in patients with symptomatic KOA taking either IATH or placebo | To assess the effect of IATH on WOMAC pain score and physical global assessment vs. placebo after 4 and 12 weeks treatment | A significant improvement in WOMAC pain was observed at week 4 in IATH group but not in placebo group as compared with baseline. The effect on pain subscale scores at 12 weeks was greater in subjects with non-inflammatory rather than inflammatory synovitis |
| McAlindon et al. (2017) [19] | A 2-year RCT,140 patients with symptomatic KOA | The effect of IATH vs. saline on pain (WOMAC) and progression of cartilage loss evaluated by MRI | IATH had no significant effect on knee pain severity as compared to saline, but was associated with a significantly greater cartilage loss than placebo |
| Conaghan et al. (2018) [35] | RCT, in patients with KOA (Kellgren-Lawrence grade 2 or 3) | Efficacy of a single 40 mg microsphere-based IATH vs. normal saline on pain assessed by average-daily-pain or WOMAC | At week 12, pain reduction from baseline in IATH group was significantly greater than placebo |
| Arroll et al. (2004) [39] | Meta-analysis of 10 trials comprised 538 patients | To determine efficacy of IACS in symptomatic KOA and to identify number needed to treat | Overall, compared to control, IACS provided a short-term improvement in symptoms of KOA up to 2 weeks. A significantly longer duration (16–24 weeks) improvement also observed in studies with sound methodology. At least an equivalent dose of 50 mg prednisone was needed to achieve benefit at 16–24 weeks |
| Bannuru et al. (2009) [38] | Meta-analysis of 7 eligible trials comprised 606 patients | Comparing the effect of IACS vs. IAHA on pain were computed from baseline at 2, 4, 8, 12, and 26 week | IACS was more effective than IAHA up to week 4. By week 4, the two groups had similar efficacy, but IAHA was more effective beyond week 8 |
| Hepper et al. (2009) [21] | A systematic review of 6 trials compared corticosteroids with placebo and 4 papers which compared different steroids | To determine efficacy of treatment on pain and duration of pain relief according to type of corticosteroids | Compared with placebo corticosteroids reduced pain significantly at week 1 with mean difference of 22%. Two of 4 trials found more efficacy of IATH than other corticosteroids |
| Jüni et al. (2015) [20] | Meta-analysis of 27 RCTs with 1767 participants | To determine the effect of IACS on pain, function quality of life in KOA and its harms compared with sham treatment or no intervention in KOA patients | IACS exerted a moderate benefit at week 1, and a small benefit at week 4–13 and no benefit at week 24. Adverse effect in IACS users were less likely by 11% |
| He et al. (2017) [40] | Meta-analysis of 12 RCTs comprised 1794 patients with KOA who received treatment with ICS and IAHA over 3–6 months | Comparing efficacy of IACS and IAHA on pain relief in KOA | In IACS group reduction in VAS score was greater than IAHA group up to month 1, but s similar at month 3. IAHA was more effective in month 6. Changes in WOMAC score were similar at month 3 but IAHA showed greater relative effect at 6 months. Overall, IACS exerted greater short-term effect on pain (up to 1 month) but IHAH showed greater long-term (up to 6months) effect. The effect on function improvement was similar |
[i] HAQ – health assessment questionnaire, IACS – intra-articular corticosteroids, IAHA – intra-articular hyaluronic acid, IAMP – intra-articular methylprednisolone, IATH – intra-articular triamcinolone hexacetonide, KOA – knee osteoarthritis, KOOS – Knee Injury and Osteoarthritis Outcome Score, MRI – magnetic resonance imaging, OA – osteoarthritis, RCT – randomized controlled trial, VAS – visual analogue scale, WOMAC – Western Ontario and McMaster Universities OA Index.
Table II
Results of uncontrolled clinical trials addressed efficacy of intra-articular corticosteroids in knee osteoarthritis
| Authors (year) | Characteristics of patients, study type | Aims of studies | Results |
|---|---|---|---|
| Pyne et al. (2004) [43] | Comparative study, 57 patients with symptomatic KOA with knee effusion | To compare the effect of 20 mg IATH with 40 mg IAMP on knee pain (VAS) and, stair climb time (Lequesne index) over 8 weeks | Both drugs exhibited similar temporary pain relief at week 3. IATH was more effective at week 3 and the effect of IAMP on pain persisted up to week 8. Both drugs had no effect on function at 3 week or 8 week |
| Wenham et al. (2014) [47] | Uncontrolled clinical trials. 20 patients with clinical KOA | Efficacy of 80 mg IAMP on pain, assessed by both VAS and WOMAC and effect on synovial inflammation assessed by DCE-MRI | IACS reduced pain and synovial inflammation. STV reduced in responders but increased in non-responders. DCE-MRI was a sensitive marker of treatment response. There was a moderate association between the late enhancement ratio and both WOMAC pain score and 48 h pain VAS score |
| Lomonte et al. (2015) [44] | The intention-to-treat study of 100 patients with symptomatic KOA with Kellgren and Lawrence grade II or III | Comparing the effect of IATH and IAMP on pain assessed with VAS and function assessed with Lequesne index and global assessment of disease over 24 weeks | Both drugs were equally effective for pain and function up to 24 weeks |
| O’Neill et al. (2016) [10] | Open-label study of 120 symptomatic KOA | To determine the effect of IACS on changes in pain assessed with KOOS pain score and STV with DCE-MRI before and 20 days after IACS followed for 6 month compared to baseline | There was a significant association between changes in STV and KOOS pain score. A significant reduction in pain and STV occurred in 71%. STV shrank following steroid therapy, and rebounded in those whose pain relapsed |
| Gait et al. (2016) [48] | Uncontrolled clinical trial of 93 patients underwent DCE-MRI before and 1–2 weeks after IATH | To determine the effect of 80 mg IAMP on STV assessed with DCE-MRI and pain assessed with KOOS pain score. To determine correlation between changes in STV and changes in pain during the study period | Treatment was associated with decreased STV and decreased knee pain. Changes in knee pain was strongly and positively correlated with changes in DCE-MRI |
| Buyuk et al. (2017)[45] | Comparative prospective study of 126 patients with bilateral KOA | To compare the effect of IATH vs. IAMP on pain assessed with VAS and WOMAC at 2, 4, 8, 12, and 24 weeks post-injection | Compared to baseline both drugs exerted similar and significant efficacy in improvement of VAS and WOMAC pain scores and knee function until 24 weeks. Both knees improved similarly |
| Matzkin et al. (2017) [46] | Prospective study, 100 patients with symptomatic radiographic KOA | Efficacy of a single IACS on pain of the affected knee 3 weeks, 6 weeks and 6 months after injection | Compared to baseline WOMAC score improved at all-time points. However, obese patients with Kellgren and Lawrence grade 3 or 4 had significantly worse WOMAC scores at baseline, 6 weeks, and 3 months |
| Liu et al. (2018) [37] | Comparative case-control study. 412 patients with symptomatic knee | To determine the long-term effect of IACS and IAHA on pain, stiffness and function assessed with WOMAC over 2 years by comparison of users and non-users | IACS received by 77.2% and IAHA received by 22.8%. Taking either IACS or IAHA was not associated with reduced symptoms as compared with non-users |
| Calvet et al. (2018) [41] | 1-year prospective study,132 patients with KOA | To determine frequency of pain relief and predictors of treatment response one year after injection of 40 mg IATH at baseline and another injection one month later, and other injections as needed over 1 year after treatment | Improvement in VAS pain score observed in 61.4% of patients one year after treatment. The presence of pain and synovial fluid at month 1 were predictors of treatment response |
| Heidari et al. (2005) [12] | Open-label uncontrolled study of 71 patients with symptomatic KOA | To investigate the effect of a single 80 mg IATH on pain assessed with WOMAC functional disability assessed with Lequesne Index over 4 weeks compared with baseline | A significant improvement was observed in pain, effusion, functional capacity and physical activity as compared with baseline |
[i] DCE-MRI – dynamic contrast-enhanced magnetic resonance imaging, IACS – intra-articular corticosteroids, IAMP – intra-articular methylprednisolone, IATH – intra-articular triamcinolone hexacetonide, KOA – knee osteoarthritis, KOOS – Knee injury and Osteoarthritis Outcome Score, STV – synovial tissue volume, VAS – visual analog scale, WOMAC – Western Ontario and McMaster Universities OA Index.
Raynauld et al. [36] in a 2-year RCT of 68 patients with symptomatic KOA compared the effect of intra-articular triamcinolone hexacetonide (IATH) on pain score, night pain, range of motion and changes in joint space.
In this study repeated injections of IATH every 3 months over 2 years of the study period were safe and clinically effective on night pain and range of motion until 1 year after initiation of treatment as determined by total score on the WOMAC, physician’s global assessment, patient’s global assessment, patient’s assessment of pain, range of motion of the affected knee, and 50-foot walking time as assessed before each injection [36].
However, McAlindon et al. [19] in another RCT of patients with symptomatic KOA found no significant effect of every 3 months injections of IATH on severity of pain as compared with saline by using WOMAC osteoarthritis index collected every 3 months.
Nevertheless, 4 randomized controlled trials which assessed the effect of a single IATH or intra-articular methylprednisolone (IAMP) on knee pain and clinical symptoms of KOA, found greater improvement of pain, function, stiffness and walking time in the treatment group as compared with placebo [14, 16, 25, 34].
In one of these randomized controlled trial, a single injection of IATH resulted in improvement of pain, function health assessment questionnaire (HAQ) and walking time in 75% of patients in IATH group vs. 45% of the placebo group. However, duration of efficacy was short and treatment response was mostly observed in patients with joint effusion [16].
Several uncontrolled clinical trials have also shown efficacy of a single IACS injection on pain, stiffness, physical activities and quality of life in knee osteoarthritis (Table II) [10, 12, 23, 37, 41, 43–47].
In an uncontrolled open-label clinical trial of 71 patients with symptomatic KOA, who presented with history of knee joint swelling, effusion and night pain for at least 3 months. Four weeks after treatment with a single injection of IACS, proportion of patients with joint effusion, night pain, limitation of physical activity, and functional capacity decreased from 100%, 95%, 75%, and 80% at baseline to 5%, 2%, 25%, and 45% at endpoint respectively [12].
A comparative study which compared the effect of IACS and intra-articular hyaluronic acid (IAHA) on pain relief between users and non-users, indicated that long-term administration of one or more intra-articular injection of IACS over a 2-year follow-up period had no effect on knee pain, stiffness and function as compared with non-users [37]. The beneficial effects of IACS on pain, function and quality of life have been also shown in several meta-analyses [20, 21, 38–40]. In all studies improvement of symptoms in IACS group was significantly higher than the placebo group (Table I).
The average duration of pain relief or pain reduction in RCTs and meta-analyses, as well as in uncontrolled clinical trials varied from 1 or 2 weeks to as long as 3–24 weeks [10, 12, 42–46].
Sample size, duration of treatment, sensitivity of outcome measures, and type of treatment outcome can differently affect the results and limit detection of real difference across studies, as well as between the treatment and placebo group [14]. Furthermore, inaccessibility to synovial fluid during injection, and inadequate joint aspiration prior to injection of IACS can lead to insufficient treatment response and underestimation of IACS effect [16].
Effect on structural changes
A few studies have addressed the effect of IACS on progression of KOA (Table I and II). The results of two 2-year RCTs which have assessed the effect of IACS on structural changes in KOA were inconsistent [19, 36].
In one study repeated injections of IATH every 3 months was safe without any effect on radiographic joint space narrowing progression after 2 years [36], while, McAlindon et al. [19] in another 2-year RCT found significantly greater MRI detected cartilage volume loss in IATH treated patients as compared with placebo.
Contradictory results may be explained by lower sensitivity of radiography than MRI in detecting small structural changes. However, none of these studies assessed changes in synovial tissue volume (STV) or severity of synovitis, which is the main cause of structural changes and progression [4, 10, 16, 34, 47, 48].
O’Neill et al. [10] in a prospective study of 120 symptomatic KOA found significant reduction of STV after an injection of 80 mg IAMP. Compared with baseline, STV reduction was shown by dynamic contrast-enhanced magnetic resonance imaging (DCE-MRI) in 71% of patients after a median duration of 8 days interquartile range (IQR = 7–14 days) and 23 of them (19.1%) were persistent responders at 6 months. A similar findings were found in 2 uncontrolled clinical trials after a single injection of intra-articular methylprednisolone.
In these studies, compared with baseline, STV as determined by DCE-MRI, had decreased significantly in responder patients 1–2 weeks after treatment, whereas in non-responders the value of STV increased [47, 48].
Predictors of treatment response
Identification of a clinical or imaging findings to predict response to IACS therapy in KOA was the topic of many RCTs and meta-analyses as well as a number of uncontrolled clinical studies. A few clinical or imaging parameters have been found to yield predictive ability (Table III and Table IV).
Table III
Randomized controlled trials and meta-analyses studies addressed predictors of response to intra-articular corticosteroids in knee osteoarthritis
| Authors (year) | Type and purpose of studies | Treatment outcomes | Predictors of response to treatment |
|---|---|---|---|
| Gaffney et al. (1995) [16] | Uncontrolled clinical trial in 84 patients with KOA | Clinical improvement | Presence of joint effusion, joint aspiration predicted outcome |
| Jones et al. (1996) [14] | RCT of 59 patients with symptomatic KOA | A significant short-term reduction in knee pain as compared with placebo group | No clinical predictor was found |
| Chao et al. (2010) [34] | RCT of 40 mg IATH vs. placebo in 79 patients with symptomatic KOA | Short duration of pain relief (4–12 weeks) | Non-inflammatory synovial hypertrophy |
| Hirsch et al. (2013) [55] | A meta-analysis of 21 studies | Identification of a predictor response | No predictor was found based on radiographic findings, clinical or sonographic evidence of inflammation or synovial hypertrophy |
| Maricar et al. (2013) [49] | A meta-analysis of 11 studies | To address clinical efficacy of treatment | Presence of effusion, baseline severity of symptoms |
Table IV
Uncontrolled clinical studies which addressed predictors of response to intra-articular corticosteroids in knee osteoarthritis
| Authors (year) | Type and purpose of studies | Treatment outcomes | Predictors of response to treatment |
|---|---|---|---|
| Pendelton et al. (2008) [42] | Study of 86 patients with KOA | Clinical improvement in 70% of participants | No predictor, including no predictive ability of ultrasound-detected synovitis |
| Wenham et al. (2014) [47] | 20 KOA treated with 80 mg IAMP | Reduction of pain and synovial volume | Presence of synovitis |
| O’Neill et al. (2016) [10] | Open-label prospective study, efficacy of 80 mg IAMP | Reduction in pain and STV. A significant association between change in the level of STV and change in level of pain | Synovitis |
| Fatimah et al. (2016) [54] | 174 patients with KOA who received IACS | Improvement of pain > 50 % compared to baseline | Age, range of movement, local knee tenderness radiographic score |
| Matzkin et al. (2017) [46] | Prospective study of 100 patients with symptomatic KOA | Clinical improvement of pain | Radiographic scores of grades 1 and 2 Kellgren and Lawrence |
| McCabe et al. (2017) [51] | Open-label study of patients with symptomatic KOA treated with 80 mg IAMP | To determine relationship between SF-WBC count with pain and KOA severity | Higher number of total SF-WBC was predictor of treatment response |
| Miletic et al. (2018) [52] | Prospective outcomes study of 117 patients with KOA | Clinical improvement at all-time points | Radiographic changes at grade 2 OARSI |
| Maricar et al. (2017) [53] | Open-label study of 207 patients with KOA | Evaluation of treatment response | Severity of cartilage damages |
| Bevers et al. (2014) [50] | 62 patients with KOA | Pain reduction in 62% of study population | Synovitis detected by DCE-MRI |
| Gait et al. (2016) [48] | A clinical study of 93 patients with KOA | An association between changes in pain and synovitis | synovitis detected by DCE-MRI |
[i] DCE-MRI – dynamic contrast-enhanced magnetic resonance imaging, IACS – intra-articular corticosteroids, IAMP – intra-articular methylprednisolone, IATH – intra-articular triamcinolone hexacetonide, KOA – knee osteoarthritis, OARSI – Osteoarthritis Research Society International, SF-WBC – synovial fluid white blood cell count, STV – synovial tissue volume.
A relationship between synovitis with pain, swelling, effusion, and cartilage destruction [4, 10, 16, 34, 47, 48] suggests synovitis as a target for treatment as well as a parameter in predicting treatment response. Predictive accuracy of other parameters such as the presence of joint effusion, severity of symptoms at baseline, even predictive performance of just joint fluid aspiration alone, has been also investigated in a few studies [16, 49].
In 3 clinical trials, the presence of synovitis was a predictor of treatment response, and improvement of synovitis as detected by either ultrasound or MRI was significantly associated with reduction of knee pain [10, 34, 49].
In a recent 1-year prospective study of 132 patients with KOA the presence of pain or ultrasound-detected joint effusion one month after initiation of IACS treatment was predictor of treatment response at one year [41].
In contrast in an uncontrolled study neither synovitis nor effusion was predictor of treatment response, but higher scores of pain and the presence of patellar tendinopathy at baseline were predictors of significant improvement. In this study 68% of patients had synovitis and 46% had joint effusion in clinical examination, and musculoskeletal ultrasound detected synovitis and effusion were found in 79 % and 62% of patients respectively [42].
Similarly, in another prospective study by Bevers et al. [50] ultrasound-detected synovitis was not predictor of pain relief. This issue may indicate the existence of synovitis could not be detected by using current diagnostic methods or pain reduction in KOA is not related to suppression of synovitis alone. Higher number of synovial fluid white blood cells (SF-WBC) was predictor of treatment response in one study of patients with symptomatic knee osteoarthritis. In this study a single 80 mg IAMP injection in subjects with higher total SF-WBC count was associated with greater pain reduction [51].
In some studies lower structural damages, age, local tenderness were predictors of treatment response [46, 52, 53]. In many studies no predictors were detected and even, the presence of synovitis was not predictor of treatment response [14, 46, 52–54]. In a meta-analysis of 21 studies by Hirsch et al. [55] none of clinical, sonographic or radiographic features of KOA were predictor of treatment response.
Nonetheless, Maricar et al. [49] in a meta-analysis of 11 studies found an association of treatment response with several parameters such as, joint effusion, joint fluid withdrawal, severity of disease, absence of synovitis, baseline severity, accuracy of intra-articular injection of corticosteroid. In this study identification of a specific predictor was impossible.
Safety of intra-articular corticosteroids in knee osteoarthritis
Long-term safety of IACS therapy in symptomatic KOA has been shown in 2 meta-analyses [20, 39]. In these studies adverse effects in the treatment and placebo groups were similar. In one meta-analysis local adverse effect in IACS group was lower than in IAHA group [39]. The safety of IACS has been also addressed in 2 RCTs [19, 36].
Raynauld et al. [36] found no deleterious anatomical structures changes despite of clinical improvement in patients taking repeated IACS every 3 months over 2 years of the study period.
By contrast, McAlindon et al. [19] in another RCT, found that repeated IACS every 3 months was associated with greater cartilage volume loss without any beneficial effect. Two observational studies [56, 57] found and association between IACS and progression of knee osteoarthritis.
However, the results of latter studies in assigning radiographic progression to IACS alone are limited because, several factors such as retrospective study design, patients selection, self-reported data regarding the type, time and number of IACS could confound the results.
Furthermore, patients with and without progressions have not been matched regarding baseline severity of osteoarthritis, as well as many associated factors of osteoarthritis progression. In addition, the safety outcome was not the primary objective of these studies.
The results of a meta-analysis of 40 studies which reviewed current literature on the effect of IACS on articular cartilage, supported the beneficial effects of IACS administration in knee osteoarthritis. In this study the impact of IACS on articular cartilage was time-and-dose dependent.
The beneficial effects were observed in studies with low doses of steroids and short duration of treatment, whereas high doses and long-term IACS therapy were associated with detrimental effects [58].
Overall, using intra-articular corticosteroids in KOA is relatively safe for short-term period, but its long-term effects on articular cartilage and other joint structures are unknown and remain to be determined [59].
Limitations
This study has several limitations, because, the studies included in this review were different in respect to study design, study population, patients characteristics, severity of structural damages, dosage of IACS, number of injections, duration of follow-up, treatment outcome and measures applied for assessment of treatment efficacy. In particular, the presence or absence of synovial inflammation and the method of diagnosis of synovitis is important. These factors can differently affect the results of treatment across studies.
Osteoarthritis is a multifactorial disease with heterogeneous phenotypes in terms of clinical manifestations and etiologies. Hence, knee osteoarthritis patients are classified to subgroups according to structural, etiological and epidemiological phenotypes. This classification system is helpful to identify a specific subgroup of patients who display inflammatory characteristics and thus may gain more benefit from anti-inflammatory treatment [60].
Therefore, in each study population response to treatment is expected to vary according to the etiology and structural changes, the presence or absence of risk factors. Clinical trials which were included in meta-analyses also differed in respect to study design, sample size, duration of study, statistic power and outcomes measures.
A number of clinical trial may lack important covariates or data which are necessary for detection of a significant differences in meta-analysis. These factors and many unknown confounding variables should be considered in confronting with controversies across different studies.
The main purpose of treatment in KOA is improvement of pain and function through suppression of synovial inflammation, and IACS is expected to affect only on anti-inflammatory component of pain [8].
As a results in subjects with advanced radiological KOA or in patients with coexistent associated factors of KOA progression efficacy of IACS is lower as compared with those who had mild disease without risk factors.
Conclusions
Existing data indicate that intra-articular corticosteroids in knee osteoarthritis provides a short-term pain relief and functional improvement which may last from one to several weeks.
At present, synovitis is the most important predictor of treatment response, and also a target for anti-inflammatory treatment for intra-articular corticosteroids. Hence, subgroup of patients with inflammatory phenotype with clinical features of pain, stiffness joint swelling and effusion are expected to be more responsive than other phenotypes who do not display clinical manifestations of inflammation.
Nonetheless, identification of responder from non-responder patients is challenging because, inflammatory presentation of KOA is temporal and is not present at all stages of the KOA process.
At present, patients with significant disability or advanced KOA who are non-responsive to standard therapy are considered for treatment with intra-articular corticosteroids.
Inefficiency of intra-articular corticosteroids in these patients is predictable, because in these subgroups, synovitis alone is not the cause of pain, but structural changes, mechanical and anatomical factors, and even extraarticular factors are also responsible, thus suppression of synovial inflammation by using IACS is likely to provide a short-term pain relief or no therapeutic benefit.
This issue is important, in particular patients who are expected to be respondent to IACS needs to be selected among population of KOA who have synovial inflammation with minimal or moderate anatomical abnormalities. Suppression of inflammatory process at early stages of KOA in addition to pain relief and functional improvement may prevent progression of structural changes.
Given an anti-inflammatory and chondroprotective properties of corticosteroids, the goals of future clinical trials should not be limited to short-term pain relief, but also prevention of osteoarthritis progression by identification of patients who not only have synovitis but they are also at higher risk of disease progression.