Current issue
Archive
Online first
About the Journal
Editorial Office
Editorial Board
Publisher
Editorial Policies
Ethical standards and procedures
Abstracting and indexing
Reviewers
Honorary Reviewers
Subscription
Contact
Most read articles
Instructions for authors
Article processing charge (APC)
Books and Events
Books
Events
ORIGINAL PAPER
Clinical and laboratory differences in characteristics of patients with early-onset and late-onset systemic lupus erythematosus: a single-center retrospective study
1
Doctoral School of Medical and Health Sciences, Jagiellonian University Medical College, Krakow, Poland
2
Clinical Department of Rheumatology, Immunology and Internal Medicine, University Hospital in Krakow, Poland
3
Faculty of Exact and Technical Science, Institute of Computer Science, University of Rzeszow, Poland
4
Department of Dermatology, Jagiellonian University Medical College, Krakow, Poland
5
Department of Internal Medicine, Faculty of Medicine, Jagiellonian University Medical College, Krakow, Poland
6
Department of Rheumatology and Immunology, Jagiellonian University Medical College, Krakow, Poland
Submission date: 2025-03-25
Final revision date: 2025-06-03
Acceptance date: 2025-07-11
Online publication date: 2026-03-23
Corresponding author
Joanna Kosałka-Węgiel
Department of Rheumatology and Immunology, Jagiellonian University Medical College, 2 Jakubowskiego St., 30-688 Krakow, Poland
Department of Rheumatology and Immunology, Jagiellonian University Medical College, 2 Jakubowskiego St., 30-688 Krakow, Poland
KEYWORDS
early-onset systemic lupus erythematosuslate-onset systemic lupus erythematosussystemic lupus erythematosusinterstitial lung diseasecomorbidities
TOPICS
ABSTRACT
Introduction:
Systemic lupus erythematosus (SLE) is a complex autoimmune disease with clinical and laboratory characteristics influenced by the age of onset. Despite its significance, data on late-onset SLE (Lo-SLE) compared to early-onset SLE (Eo-SLE) remain limited, particularly in the Polish population. We investigated differences between Lo-SLE and Eo-SLE patients (using 50 years as a cutoff), aiming to improve the diagnosis and management of SLE patients across different age groups.
Material and methods:
We conducted a retrospective analysis of medical records from all SLE patients treated at the University Hospital in Krakow, Poland, from 2012 to 2022. All included patients met the 2019 European Alliance of Associations for Rheumatology and American College of Rheumatology classification criteria for SLE.
Results:
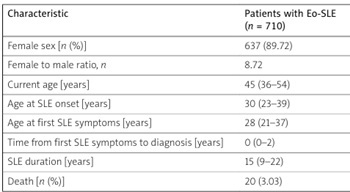
We analyzed 710 patients with Eo-SLE (77.9%) and 201 patients with Lo-SLE (22.1%). Compared to the Eo-SLE group, the Lo-SLE group exhibited shorter disease duration (p < 0.001), a higher mortality rate (p < 0.001), and distinct clinical features: less involvement of the central nervous system (n = 5, 2.5% vs. n = 51, 7.23%, p = 0.014) and kidney (n = 49, 24.38% vs. n = 294, 41.41%, p < 0.001), more frequent interstitial lung disease (n = 19, 9.45% vs. n = 27, 3.84%, p = 0.001), and a higher prevalence of cardiovascular, metabolic, and neoplastic comorbidities (p < 0.05, for all). Autoantibody profiles also differed: in Lo-SLE compared to Eo-SLE patients, anti-SSB were more common, while anti-histone, anti-nucleosome, anti-RNP, and anti-dsDNA antibodies were less prevalent. Late-onset SLE patients received immunosuppressive treatment less often than Eo-SLE patients.
Conclusions:
Late-onset SLE patients exhibit different disease manifestations but with a higher prevalence of interstitial lung disease, internal medicine comorbidities, malignancies, and cardiovascular events compared to Eo-SLE. Our findings highlight the need for tailored management strategies in elderly SLE patients.
Systemic lupus erythematosus (SLE) is a complex autoimmune disease with clinical and laboratory characteristics influenced by the age of onset. Despite its significance, data on late-onset SLE (Lo-SLE) compared to early-onset SLE (Eo-SLE) remain limited, particularly in the Polish population. We investigated differences between Lo-SLE and Eo-SLE patients (using 50 years as a cutoff), aiming to improve the diagnosis and management of SLE patients across different age groups.
Material and methods:
We conducted a retrospective analysis of medical records from all SLE patients treated at the University Hospital in Krakow, Poland, from 2012 to 2022. All included patients met the 2019 European Alliance of Associations for Rheumatology and American College of Rheumatology classification criteria for SLE.
Results:
We analyzed 710 patients with Eo-SLE (77.9%) and 201 patients with Lo-SLE (22.1%). Compared to the Eo-SLE group, the Lo-SLE group exhibited shorter disease duration (p < 0.001), a higher mortality rate (p < 0.001), and distinct clinical features: less involvement of the central nervous system (n = 5, 2.5% vs. n = 51, 7.23%, p = 0.014) and kidney (n = 49, 24.38% vs. n = 294, 41.41%, p < 0.001), more frequent interstitial lung disease (n = 19, 9.45% vs. n = 27, 3.84%, p = 0.001), and a higher prevalence of cardiovascular, metabolic, and neoplastic comorbidities (p < 0.05, for all). Autoantibody profiles also differed: in Lo-SLE compared to Eo-SLE patients, anti-SSB were more common, while anti-histone, anti-nucleosome, anti-RNP, and anti-dsDNA antibodies were less prevalent. Late-onset SLE patients received immunosuppressive treatment less often than Eo-SLE patients.
Conclusions:
Late-onset SLE patients exhibit different disease manifestations but with a higher prevalence of interstitial lung disease, internal medicine comorbidities, malignancies, and cardiovascular events compared to Eo-SLE. Our findings highlight the need for tailored management strategies in elderly SLE patients.
REFERENCES (27)
1.
Hoi A, Igel T, Mok CC, Arnaud L. Systemic lupus erythematosus. Lancet 2024; 403: 2326–2338, DOI: 10.1016/S0140-6736(24)-00398-2.
2.
Lisnevskaia L, Murphy G, Isenberg D. Systemic lupus erythematosus. Lancet 2014; 384: 1878–1888, DOI: 10.1016/S0140-6736(14)60128-8.
3.
Wach A, Korkosz M, Okoń K, Kosałka-Węgiel J. A case of systemic lupus erythematosus with antineutrophil cytoplasmic antibodies positive skin vasculitis and concomitant combined thrombophilia. Pol Arch Intern Med 2024; 134: 16810, DOI: 10.20452/pamw.16810.
4.
Celińska-Löwenhoff M, Musiał J. Late-onset systemic lupus erythematosus: clinical manifestations, course, and prognosis. Pol Arch Intern Med 2015; 125: 497–499.
5.
Mruthyunjaya P, Ahmed S, Botabekova A, et al. Late-onset Systemic Lupus Erythematosus. Rheumatol Int 2025; 45: 29, DOI: 10.1007/s00296-024-05784-1.
6.
Riveros Frutos A, Holgado S, Sanvisens Bergé A, et al. Late-onset versus early-onset systemic lupus: characteristics and outcome in a national multicentre register (RELESSER). Rheumatology (Oxford) 2021; 60: 1793–1803, DOI: 10.1093/rheumatology/keaa477.
7.
Piga M, Tselios K, Viveiros L, et al. Clinical patterns of disease: From early systemic lupus erythematosus to late-onset disease. Best Pract Res Clin Rheumatol 2023; 37: 101938, DOI: 10.1016/j.berh.2024.101938.
8.
Aljohani R, Gladman DD, Su J, Urowitz MB. Disease evolution in late-onset and early-onset systemic lupus erythematosus. Lupus 2017; 26: 1190–1196, DOI: 10.1177/0961203317696593.
9.
Jeleniewicz R, Suszek D, Majdan M. Clinical picture of late-onset systemic lupus erythematosus in a group of Polish patients. Pol Arch Intern Med 2015; 125: 538–544, DOI: 10.20452/pamw.2963.
10.
Aringer M. EULAR/ACR classification criteria for SLE. Semin Arthritis Rheum 2019; 49 (Suppl 3): S14–S17, DOI: 10.1016/j.semarthrit.2019.09.009.
11.
Kosałka-Węgiel J, Dziedzic R, Siwiec-Koźlik A, et al. Clinical and laboratory characteristics of early-onset and delayed-onset lupus nephritis patients: a single-center retrospective study. Rheumatol Int 2024; 44: 1283–1294, DOI: 10.1007/s00296-024-05579-4.
12.
The American College of Rheumatology nomenclature and case definitions for neuropsychiatric lupus syndromes. Arthritis Rheum 1999; 42: 599–608, DOI: 10.1002/1529-0131(199904)42:4<599::AID-ANR2>3.0.CO;2-F.
13.
Alonso MD, Llorca J, Martinez-Vazquez F, et al. Systemic Lupus Erythematosus in Northwestern Spain: A 20-Year Epidemiologic Study. Medicine (Baltimore) 2011; 90: 350–358, DOI: 10.1097/MD.0b013e31822edf7f.
14.
Bindroo MA, Majid N, Ekbote G, et al. Late Onset Systemic Lupus Erythematosus – Clinical and Autoantibody Profile and its Comparison with Young Onset Systemic Lupus Erythematosus. Mediterr J Rheumatol 2023; 34: 454–459, DOI: 10.31138/mjr.290723.los.
15.
Medlin JL, Hansen KE, McCoy SS, Bartels CM. Pulmonary manifestations in late versus early systemic lupus erythematosus: A systematic review and meta-analysis. Semin Arthritis Rheum 2018; 48: 198–204, DOI: 10.1016/j.semarthrit.2018.01.010.
16.
Catoggio LJ, Soriano ER, Imamura PM, et al. Late-onset systemic lupus erythematosus in Latin Americans: a distinct subgroup? Lupus 2015; 24: 788–795, DOI: 10.1177/0961203314563134.
17.
Luppi F, Sebastiani M, Silva M, et al. Interstitial lung disease in Sjögren’s syndrome: a clinical review. Clin Exp Rheumatol 2020; 38 Suppl 126: 291–300.
18.
Pamuk ON, Raza AA, Hasni S. Neuropsychiatric lupus in late- and early-onset systemic lupus erythematosus patients: a systematic review and meta-analysis. Rheumatology 2024; 63: 8–15, DOI: 10.1093/rheumatology/kead297.
19.
Maddison P, Farewell V, Isenberg D, et al.; Systemic Lupus International Collaborating Clinics. The rate and pattern of organ damage in late onset systemic lupus erythematosus. J Rheumatol 2002; 29: 913–917.
20.
Kosałka-Węgiel J, Pacholczak-Madej R, Dziedzic R, et al. Malignancy in systemic lupus erythematosus: relation to disease characteristics in 92 patients – a single center retrospective study. Rheumatol Int 2024; 44: 1701–1713, DOI: 10.1007/s00296-024-05623-3.
21.
Dong Z, Hou L, Luo W, et al. Myocardial infarction drives trained immunity of monocytes, accelerating atherosclerosis. Eur Heart J 2024; 45: 669–684, DOI: 10.1093/eurheartj/ehad787.
22.
Mahir L, Ezzahra Hsai F, Drissi Bourhanbour A, El Bakkouri J. Performance evaluation of immunoblot for the detection of anti-DNA antibodies compared to indirect immunofluorescence on Crithidia luciliae. J Hum Virol Retrovirol 2023; 10: 30–32.
23.
Padovan M, Govoni M, Castellino G, et al. Late onset systemic lupus erythematosus: no substantial differences using different cut-off ages. Rheumatol Int 2007; 27: 735–741, DOI: 10.1007/s00296-006-0284-3.
24.
Fanouriakis A, Kostopoulou M, Alunno A, et al. 2019 update of the EULAR recommendations for the management of systemic lupus erythematosus. Ann Rheum Dis 2019; 78: 736–745, DOI: 10.1136/annrheumdis-2019-215089.
25.
Fireman M, DiMartini AF, Armstrong SC, Cozza KL. Immunosuppressants. Psychosomatics 2004; 45: 354–360, DOI: 10.1176/appi.psy.45.4.354.
26.
Rodrigues MCS, Oliveira CD. Drug-drug interactions and adverse drug reactions in polypharmacy among older adults: an integrative review. Rev Lat Am Enfermagem 2016; 24: e2800, DOI: 10.1590/1518-8345.1316.2800.
27.
Viveiros L, Neves A, Gouveia T, Isenberg DA. A large cohort comparison of very late-onset systemic lupus erythematosus with younger-onset patients. Clin Exp Rheumatol 2024; 42: 1480–1486, DOI: 10.55563/clinexprheumatol/jgsyos.
Copyright: © Narodowy Instytut Geriatrii, Reumatologii i Rehabilitacji w Warszawie. This is an Open Access journal, all articles are distributed under the terms of the Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International (CC BY-NC-SA 4.0) License (https://creativecommons.org/licenses/by-nc-sa/4.0/), allowing third parties to copy and redistribute the material in any medium or format and to remix, transform, and build upon the material, provided the original work is properly cited and states its license.
Share
RELATED ARTICLE
We process personal data collected when visiting the website. The function of obtaining information about users and their behavior is carried out by voluntarily entered information in forms and saving cookies in end devices. Data, including cookies, are used to provide services, improve the user experience and to analyze the traffic in accordance with the Privacy policy. Data are also collected and processed by Google Analytics tool (more).
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.