Current issue
Archive
Online first
About the Journal
Editorial Office
Editorial Board
Publisher
Editorial Policies
Ethical standards and procedures
Abstracting and indexing
Reviewers
Honorary Reviewers
Subscription
Contact
Most read articles
Instructions for authors
Article processing charge (APC)
Books and Events
Books
Events
ORIGINAL PAPER
Effect of dry needling therapy on hip range of motion as a component of functional performance in patients with chronic low back pain: a randomized clinical trial
1
Institute of Health Sciences, University of Opole, Poland
2
Institute of Medical Sciences, University of Opole, Poland
3
Institute of Physiotherapy and Health Sciences, Academy of Physical Education, Katowice, Poland
Submission date: 2025-06-02
Final revision date: 2025-10-06
Acceptance date: 2026-01-21
Online publication date: 2026-03-06
Publication date: 2026-05-09
Corresponding author
Joanna Barbara Rajfur
Institute of Health Sciences, University of Opole, 68 Katowicka St., 45061 Opole, Poland
Institute of Health Sciences, University of Opole, 68 Katowicka St., 45061 Opole, Poland
Reumatologia 2026;64(2):124-131
KEYWORDS
TOPICS
ABSTRACT
Introduction:
The dry needling (DN) method is increasingly used in the treatment of low back pain (LBP). It involves inserting a thin needle into the tissue without anesthesia or injection. The therapeutic effect of DN is related to the change in the mechanical sensitivity of muscle tissue and reducing pain in patients with musculoskeletal dysfunctions. The aim of this study was to evaluate the effect of DN according to the Five Regulatory Systems Concept (FRSc) on the range of motion of the hip joints as a component of functional performance in patients with chronic LBP.
Material and methods:
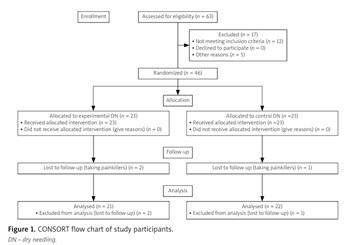
The study included 46 patients with LBP assigned to the experimental group (n = 23, DN + rehabilitation) or control group (n = 23, DN sham + rehabilitation). Both groups underwent a total of 8 treatments, performed twice a week for 4 weeks (a single treatment lasted 60 minutes). An electronic goniometer was used to assess the range of motion of the hip joints. Measurements were taken before and immediately after the intervention and at 1-month and 3-month follow-up.
Results:
In the measurements of the range of hip movement for both lower limbs in both groups there were statistically significant differences (main effect: p < 0.05). In the study group, the final improvement for the right limb was by 12.3 points (p < 0.001), for the left by 10 points (p < 0.001). In the control group, improvement was noted immediately after the completed therapy, for the right limb by 15 points (p < 0.001), for the left by 18 points (p = 0.334). In 3-month observation, the effects proved unstable.
Conclusions:
The use of DN according to the FRSc contributes to improved hip range of motion in patients with LBP. When used in conjunction with an exercise program, it can be an effective adjunct to standard physiotherapy for patients with LBP.
The dry needling (DN) method is increasingly used in the treatment of low back pain (LBP). It involves inserting a thin needle into the tissue without anesthesia or injection. The therapeutic effect of DN is related to the change in the mechanical sensitivity of muscle tissue and reducing pain in patients with musculoskeletal dysfunctions. The aim of this study was to evaluate the effect of DN according to the Five Regulatory Systems Concept (FRSc) on the range of motion of the hip joints as a component of functional performance in patients with chronic LBP.
Material and methods:
The study included 46 patients with LBP assigned to the experimental group (n = 23, DN + rehabilitation) or control group (n = 23, DN sham + rehabilitation). Both groups underwent a total of 8 treatments, performed twice a week for 4 weeks (a single treatment lasted 60 minutes). An electronic goniometer was used to assess the range of motion of the hip joints. Measurements were taken before and immediately after the intervention and at 1-month and 3-month follow-up.
Results:
In the measurements of the range of hip movement for both lower limbs in both groups there were statistically significant differences (main effect: p < 0.05). In the study group, the final improvement for the right limb was by 12.3 points (p < 0.001), for the left by 10 points (p < 0.001). In the control group, improvement was noted immediately after the completed therapy, for the right limb by 15 points (p < 0.001), for the left by 18 points (p = 0.334). In 3-month observation, the effects proved unstable.
Conclusions:
The use of DN according to the FRSc contributes to improved hip range of motion in patients with LBP. When used in conjunction with an exercise program, it can be an effective adjunct to standard physiotherapy for patients with LBP.
REFERENCES (28)
1.
Dunning J, Butts R, Mourad F, et al. Dry needling: a literature review with implications for clinical practice guidelines. Phys Ther Rev 2014; 19: 252–265, DOI: 10.1179/108331913X13844245102034.
2.
Halle JS, Halle RJ. Pertinent dry needling considerations for minimizing adverse effects – part two. Int J Sports Phys Ther 2016; 11: 810–819.
3.
Kearns G, Fernández-De-Las-Peñas C, Brismée JM, et al. New perspectives on dry needling following a medical model: are we screening our patients sufficiently? J Man Manip Ther 2019; 27: 172–179, DOI: 10.1080/10669817.2019.1567011.
4.
Lázaro-Navas I, Lorenzo-Sánchez-Aguilera C, Pecos-Martín D, et al. Immediate effects of dry needling on the autonomic nervous system and mechanical hyperalgesia: a randomized controlled trial. Int J Environ Res Public Health 2021; 18: 6018, DOI: 10.3390/ijerph18116018.
5.
Gattie E, Cleland JA, Snodgrass S. The effectiveness of trigger point dry needling for musculoskeletal conditions by physical therapists: a systematic review and meta-analysis. J Orthop Sports Phys Ther 2017; 47: 133–149, DOI: 10.2519/jospt.2017.7096.
6.
Martín-Corrales C, Bautista IV, Méndez-Mera JE, et al. Benefits of adding gluteal dry needling to a four-week physical exercise program in a chronic low back pain population. A randomized clinical trial. Pain Med 2020; 21: 2948–2957, DOI: 10.1093/pm/pnaa279.
7.
Tüzün EH, Gıldır S, Angın E, et al. Effectiveness of dry needling versus a classical physiotherapy program in patients with chronic low-back pain: a single-blind, randomized, controlled trial. J Phys Ther Sci 2017; 29: 1502–1509, DOI: 10.1589/jpts.29.1502.
8.
Téllez-García M, de-la-Llave-Rincón AI, Salom-Moreno J, et al. Neuroscience education in addition to trigger point dry needling for the management of patients with mechanical chronic low back pain: a preliminary clinical trial. J Bodyw Mov Ther 2015; 19: 464–472. DOI: 10.1016/j.jbmt.2014.11.012.
9.
Lara-Palomo IC, Gil-Martínez E, López-Fernández MD, et al. Efficacy of dry needling for chronic low back pain: a systematic review and meta-analysis of randomized controlled trials. Altern Ther Health Med 2023; 29: 110–120.
10.
Liu L, Huang QM, Liu QG, et al. Evidence for dry needling in the management of myofascial trigger points associated with low back pain: a systematic review and meta-analysis. Arch Phys Med Rehabil 2018; 99: 144–152.e2, DOI: 10.1016/ j.apmr.2017.06.008.
11.
Funk MF, Frisina-Deyo AJ. Dry needling for spine related disorders: a scoping review. Chiropr Man Therap 2020; 28: 23, DOI: 10.1186/s12998-020-00310-z.
12.
Padanilam SJ, Dayton SR, Jarema R, et al. Dry needling for the treatment of musculoskeletal ailments with trigger points. Video J Sports Med 2021; 1: 26350254211023776, DOI: 10.1177/26350254211023776.
13.
Rajfur J, Rajfur-Stach K. Selected needling techniques in pain associated with musculoskeletal disorders: a narrative review. Med Sci Pulse 2022; 16: 57–65, DOI: 10.5604/01.3001.0015.8247.
14.
Rajfur J, Rajfur K, Kosowski Ł, et al. The effectiveness of dry needling in patients with chronic low back pain: a prospective, randomized, single-blinded study. Sci Rep 2022; 12: 15803, DOI: 10.1038/s41598-022-19980-1.
15.
Rajfur J, Rajfur K, Matusz T, et al. Dry needling with the use of FRSc technique in addition to standard rehabilitation program for chronic low back pain: a randomized controlled trial using both PROMs and measurement tools. J Pain Res 2024; 17: 1041–1053, DOI: 10.2147/JPR.S450119.
16.
Mahmoudzadeh A, Rezaeian ZS, Karimi A, Dommerholt J. The effect of dry needling on the radiating pain in subjects with discogenic low-back pain: a randomized control trial. J Res Med Sci 2016; 21: 86, DOI: 10.4103/1735-1995.192502.
17.
Deshpande AN, Lawange SA. Evaluation of effectiveness of dry needling in the treatment of chronic low back pain: A retrospective analysis. Indian J Pain 2021; 35: 141–145.
18.
Dach F, Ferreira KS. Treating myofascial pain with dry needling: a systematic review for the best evidence-based practices in low back pain. Arq Neuropsiquiatr 2023; 81: 1169–1178, DOI: 10.1055/s-0043-1777731.
19.
Khan K, Ahmad A, Mohseni Bandpei MA, Kashif M. Comparison of the effects of dry needling and spinal manipulative therapy versus spinal manipulative therapy alone on functional disability and endurance in patients with nonspecific chronic low back pain: An experimental study. Medicine (Baltimore) 2024; 103: e39734, DOI: 10.1097/MD.0000000000039734.
20.
Pecos-Martín D, Romero-Morales C, Barrero-Sánchez A, et al. Optimizing dry needling for chronic low back pain: a novel approach to treatment site selection: a randomized controlled trial. J Bodyw Mov Ther 2024; 40: 2113–2119, DOI: 10.1016/ j.jbmt.2024.10.051.
21.
Ceballos-Laita L, Estébanez-de-Miguel E, Jiménez-Rejano JJ, et al. The effectiveness of hip interventions in patients with low-back pain: a systematic review and meta-analysis. Braz J Phys Ther 2023; 27: 100502, DOI: 10.1016/j.bjpt.2023.100502.
22.
Pizol GZ, Miyamoto GC, Cabral CMN. Hip biomechanics in patients with low back pain, what do we know? A systematic review. BMC Musculoskelet Disord 2024; 25: 415, DOI: 10.1186/s12891-024-07463-5.
23.
Miyachi R, Sano A, Tanaka N, et al. Relationships among lumbar hip motion angle, perceptual awareness, and low back pain in young adults. J Phys Ther Sci 2021; 33: 880–886, DOI: 10.1589/jpts.33.880.
24.
Prather H, van Dillen L. Links between the hip and the lumbar spine (hip spine syndrome) as they relate to clinical decision making for patients with lumbopelvic pain. PM R 2019; 11 Suppl 1: S64–S72, DOI: 10.1002/pmrj.12187.
25.
Sadeghisani M, Manshadi FD, Kalantari KK, et al. Correlation between hip rotation range-of-motion impairment and low back pain. A literature review. Ortop Traumatol Rehabil 2015; 17: 455–462, DOI: 10.5604/15093492.1186813.
26.
Tanaka S, Matsumoto S, Fujii K, et al. Factors related to low back pain in patients with hip osteoarthritis. J Back Musculoskelet Rehabil 2015; 28: 409–414, DOI: 10.3233/BMR-140535.
27.
Yu Q, Chen K, Guo Z, et al. Effect of different injury morphology of the endplate on intervertebral disc degeneration: retrospective cohort study. Orthop Surg 2024; 16: 2995–3005, DOI: 10.1111/os.14238.
28.
Coskun Benlidayi I, Tirasci E. The effect of lumbosacral transitional vertebra on lumbar spine degeneration and spondylolisthesis among patients with low back pain. Pain Pract 2024; 24: 52–61, DOI: 10.1111/papr.13280.
Copyright: © Narodowy Instytut Geriatrii, Reumatologii i Rehabilitacji w Warszawie. This is an Open Access journal, all articles are distributed under the terms of the Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International (CC BY-NC-SA 4.0) License (https://creativecommons.org/licenses/by-nc-sa/4.0/), allowing third parties to copy and redistribute the material in any medium or format and to remix, transform, and build upon the material, provided the original work is properly cited and states its license.
Share
RELATED ARTICLE
We process personal data collected when visiting the website. The function of obtaining information about users and their behavior is carried out by voluntarily entered information in forms and saving cookies in end devices. Data, including cookies, are used to provide services, improve the user experience and to analyze the traffic in accordance with the Privacy policy. Data are also collected and processed by Google Analytics tool (more).
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.