Current issue
Archive
Online first
About the Journal
Editorial Office
Editorial Board
Publisher
Editorial Policies
Ethical standards and procedures
Abstracting and indexing
Reviewers
Honorary Reviewers
Subscription
Contact
Most read articles
Instructions for authors
Article processing charge (APC)
Books and Events
Books
Events
ORIGINAL PAPER
Serum low-density lipoprotein and synovial vascularity in patients with active rheumatoid arthritis and psoriatic arthritis
1
Early Arthritis Clinic, National Institute of Geriatrics, Rheumatology, and Rehabilitation, Warsaw, Poland
2
Department of Rheumatology, National Institute of Geriatrics, Rheumatology, and Rehabilitation, Warsaw, Poland
Submission date: 2025-07-14
Final revision date: 2025-09-28
Acceptance date: 2025-10-16
Publication date: 2026-04-28
Corresponding author
Reumatologia 2026;64(2):77-82
KEYWORDS
TOPICS
ABSTRACT
Introduction:
The relationship between lipid metabolism and inflammatory activity in rheumatoid arthritis (RA) and psoriatic arthritis (PsA) remains unclear. This study evaluated whether serum low-density lipoprotein cholesterol (LDL-C) levels are associated with synovial vascularization measured by quantitative power Doppler ultrasonography (PDUS) in patients with active RA and PsA.
Material and methods:
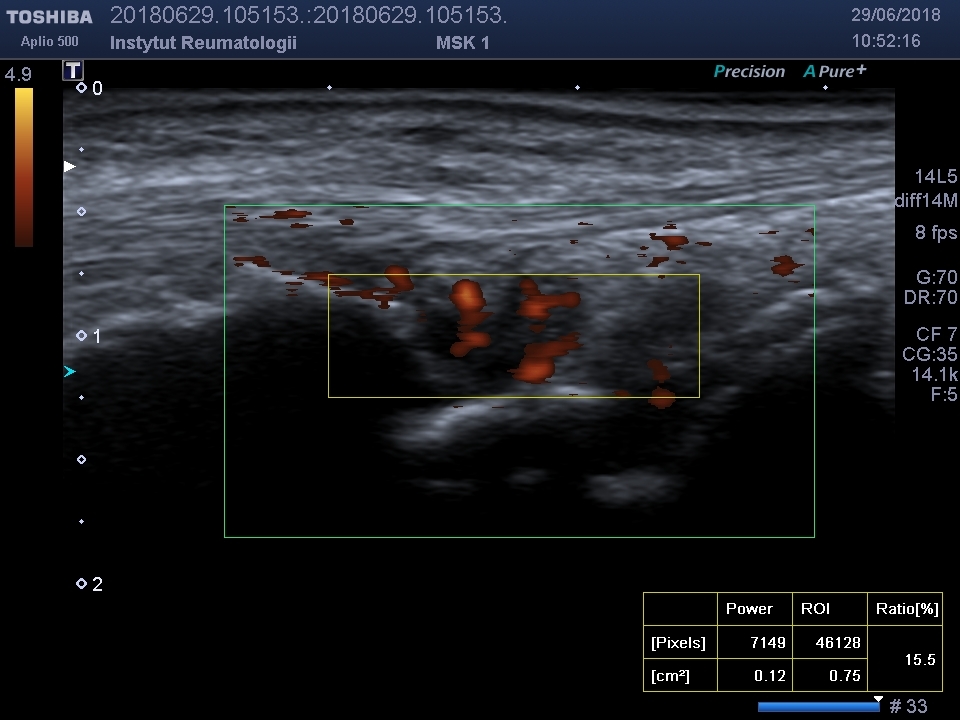
The single-center study enrolled 60 patients diagnosed with RA and a group of 20 patients with PsA with the clinical presentation resembling RA. Serum LDL-C levels were measured, and disease activity was assessed using the Disease Activity Score in 28 joints with erythrocyte sedimentation rate and the Simplified Disease Activity Index. Synovial membrane vascularization was quantified using PDUS, and a vascularity index – the PDUS index (INDEX%) – was calculated in the region of interest.
Results:
No significant correlation was found between serum LDL-C concentration and INDEX% for both groups (r = 0.2). The majority of patients in both groups (76.2%) had LDL-C levels in the normal range, consistent with the lipid paradox in inflammation.
Conclusions:
Serum LDL-C levels were not correlated with INDEX%. These findings suggest that LDL-C levels do not significantly influence synovial membrane vascularization in patients with active RA or PsA.
The relationship between lipid metabolism and inflammatory activity in rheumatoid arthritis (RA) and psoriatic arthritis (PsA) remains unclear. This study evaluated whether serum low-density lipoprotein cholesterol (LDL-C) levels are associated with synovial vascularization measured by quantitative power Doppler ultrasonography (PDUS) in patients with active RA and PsA.
Material and methods:
The single-center study enrolled 60 patients diagnosed with RA and a group of 20 patients with PsA with the clinical presentation resembling RA. Serum LDL-C levels were measured, and disease activity was assessed using the Disease Activity Score in 28 joints with erythrocyte sedimentation rate and the Simplified Disease Activity Index. Synovial membrane vascularization was quantified using PDUS, and a vascularity index – the PDUS index (INDEX%) – was calculated in the region of interest.
Results:
No significant correlation was found between serum LDL-C concentration and INDEX% for both groups (r = 0.2). The majority of patients in both groups (76.2%) had LDL-C levels in the normal range, consistent with the lipid paradox in inflammation.
Conclusions:
Serum LDL-C levels were not correlated with INDEX%. These findings suggest that LDL-C levels do not significantly influence synovial membrane vascularization in patients with active RA or PsA.
REFERENCES (18)
1.
Conforti A, Di Cola I, Pavlych V, et al. Beyond the joints, the extra-articular manifestations in rheumatoid arthritis. Autoimmun Rev 2021; 20: 102735, DOI: 10.1016/j.autrev.2020.102735.
2.
Lu Y, Cui X, Zhang L, et al. The Functional Role of Lipoproteins in Atherosclerosis: Novel Directions for Diagnosis and Targeting Therapy. Aging Dis 2022; 13: 491–520, DOI: 10.14336/AD.2021.0929.
3.
Jakubaszek M, Maślińska M, Kwiatkowska B. Quantitative Assessment of Synovial Vascularity Using Power Doppler Index in Rheumatoid Arthritis and Psoriatic Arthritis Patients with High Disease Activity [abstract]. Arthritis Rheumatol 2023; 75 (Suppl 9), DOI: 10.1002/art.42700.
4.
Wang Y, Wu H, Deng R. Angiogenesis as a potential treatment strategy for rheumatoid arthritis. Eur J Pharmacol 2021; 910: 174500, DOI: 10.1016/j.ejphar.2021.174500.
5.
Azuaga AB, Ramírez J, Cañete JD. Psoriatic Arthritis: Pathogenesis and Targeted Therapies. Int J Mol Sci 2023; 24: 4901, DOI: 10.3390/ijms24054901.
6.
Hiatt WR, Armstrong EJ, Larson CJ, Brass EP. Pathogenesis of the Limb Manifestations and Exercise Limitations in Peripheral Artery Disease. Circ Res 2015; 116: 1527–1539, DOI: 10.1161/CIRCRESAHA.116.303566.
7.
Linton MRF, Yancey PG, Davies SS, et al. The Role of Lipids and Lipoproteins in Atherosclerosis. [Updated 2019 Jan 3]. In: Feingold KR, Ahmed SF, Anawalt B, et al. (eds.). Endotext [Internet]. MDText.com, Inc, South Dartmouth 2000. Available at: https://www.ncbi.nlm.nih.gov/b... (Access: 10.07.2025).
8.
Zeng G, Zhang C, Song Y, et al. The potential impact of inflammation on the lipid paradox in patients with acute myocardial infarction: a multicenter study. BMC Med 2024; 22: 599, DOI: 10.1186/s12916-024-03823-z.
9.
Meng J, Bhalraam U, Merinopoulos I, et al. Cholesterol paradox for cardiac events: is age the missing link? Eur J Prev Cardiol 2024; 31 (Issue Supplement_1): zwae175.367, DOI: 10.1093/eurjpc/zwae175.367.
10.
Paukner K, Králová Lesná I, Poledne R. Cholesterol in the Cell Membrane-An Emerging Player in Atherogenesis. Int J Mol Sci 2022; 23: 533, DOI: 10.3390/ijms23010533.
11.
Kaysen GA, Ye X, Raimann JG, et al. Monitoring Dialysis Outcomes (MONDO) Initiative. Lipid levels are inversely associated with infectious and all-cause mortality: international MONDO study results. J Lipid Res 2018; 59: 1519–1528, DOI: 10.1194/jlr.P084277.
12.
Mostaza JM, Salinero-Fort MA, Cardenas-Valladolid J, et al. Pre-infection HDL-cholesterol levels and mortality among elderly patients infected with SARS-CoV-2. Atherosclerosis 2022; 341: 13–19, DOI: 10.1016/j.atherosclerosis.2021.12.009.
13.
Yan J, Yang S, Han L, et al. Dyslipidemia in rheumatoid arthritis: the possible mechanisms. Front Immunol 2023; 14: 1254753, DOI: 10.3389/fimmu.2023.1254753.
14.
Van Every H, Yang W, Su J, et al. Low-Density Lipoprotein Cholesterol and the Risk of Rheumatoid Arthritis: A Prospective Study in a Chinese Cohort. Nutrients 2022; 14: 1240, DOI: 10.3390/nu14061240.
15.
Pietrzak A, Chabros P, Grywalska E, et al. Serum lipid metabolism in psoriasis and psoriatic arthritis – an update. Arch Med Sci 2019; 15: 369–375, DOI: 10.5114/aoms.2018.74021.
16.
Oh EH, Ro YS, Kim JE. Epidemiology and cardiovascular comorbidities in patients with psoriasis: a Korean nationwide population-based cohort study. J Dermatol 2017; 44: 621–629, DOI: 10.1111/1346-8138.13761. .
17.
Gentile M, Peluso R, Di Minno MN, et al. Association between small dense LDL and sub-clinical atherosclerosis in patients with psoriatic arthritis. Clin Rheumatol 2016; 35: 2023–2029, DOI: 10.1007/s10067-016-3344-4. .
18.
Akkara Veetil BM, Matteson EL, Maradit-Kremers H, et al. Trends in lipid profiles in patients with psoriasis: a population- based analysis. BMC Dermatol 2012; 12: 20, DOI: 10.1186/1471-5945-12-20.
Copyright: © Narodowy Instytut Geriatrii, Reumatologii i Rehabilitacji w Warszawie. This is an Open Access journal, all articles are distributed under the terms of the Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International (CC BY-NC-SA 4.0) License (https://creativecommons.org/licenses/by-nc-sa/4.0/), allowing third parties to copy and redistribute the material in any medium or format and to remix, transform, and build upon the material, provided the original work is properly cited and states its license.
Share
RELATED ARTICLE
We process personal data collected when visiting the website. The function of obtaining information about users and their behavior is carried out by voluntarily entered information in forms and saving cookies in end devices. Data, including cookies, are used to provide services, improve the user experience and to analyze the traffic in accordance with the Privacy policy. Data are also collected and processed by Google Analytics tool (more).
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.