Dear Editor,
A 48-year-old-man, daily wage laborer by profession, came to the out-patient department with complaints of swelling in hands along with decreased sensation in arms and feet distal to elbow and knees, respectively, for the past 3 months. There was no associated pain. There was no history of fever, weight loss or any recent episode of infection or trauma. The patient was a regular smoker and consumed alcohol occasionally; dietary habits were normal. Family history was unremarkable.
The patient was examined and found to have non-pitting edema over the dorsum of the hands which extended beyond the joint line (Fig. 1A, 1B). There was no obvious tenderness. Deep tendon reflexes were preserved, and the rest of the motor examination was within normal limits. The patient had multiple hypopigmented macular patches over the back with overlying sensory loss (Fig. 1C). The routine investigations including complete blood count, liver and renal function tests were normal. The inflammatory parameters (erythrocyte sedimentation rate and C-reactive protein) were also within normal limits; thyroid profile and vitamin levels (to rule out nutritional deficiencies) also came back normal. Autoimmune workup was also negative for rheumatoid factor (RF), anti-citrullinated protein antibody (ACPA) and anti-nuclear antibody (ANA). Ultrasound examination showed presence of tenosynovitis.
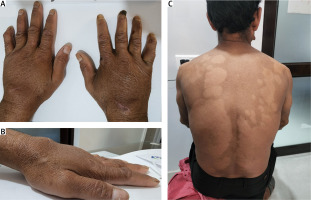
Fig. 1
Note the swelling along proximal inter-phalangeal joints, wrist and dorsum of hand in anterior and lateral view (A, B), multiple hypopigmented patches over back with sensory loss (C).
A clinical suspicion for leprosy was maintained and on thorough review of the patient, the peripheral nerves (including the ulnar nerve and common peroneal nerve) were found to be thickened and palpable. Slit skin smear was obtained to confirm the diagnosis, which showed presence of Mycobacterium leprae.
A diagnosis of multibacillary leprosy with tenosynovitis of the hands was made and the patient was started on dapsone and clofazimine daily along with rifampicin once a month (multidrug therapy). The patient gradually showed improvement with resolution of swelling and no further progression of lesions.
Leprosy is an infectious disease caused by Mycobacterium leprae that mainly affects skin and peripheral nerves. The majority of the cases are reported from India, Brazil, Bangladesh, Nepal and Indonesia [1]. Outside the endemic regions, leprosy has been reported to be associated with exposure to armadillos [2].
The disease is classified on the basis of the immune response mounted against the organism. At one end of spectrum lies tuberculoid leprosy (paucibacillary), which is characterized by a robust immune response against the bacillus and formation of granulomas and limited spread of the disease. At the other end lies lepromatous leprosy (multibacillary), which is characterized by a weak response against the bacillus resulting in disseminated disease.
Clinical manifestations include hypopigmented patches on the skin with sensory loss, collapsed nose and peripheral nerve involvement resulting in tender palpable nerves, paraesthesia and foot drop. Musculoskeletal involvement in leprosy occurs either in the form of symmetric polyarthritis mimicking rheumatoid arthritis, or it can present as tenosynovitis. Rheumatoid factor can be positive in up to 70% of patients [3]. Long standing illness can also result in Charcot’s arthropathy secondary to nerve damage.
The incidence of leprosy is declining rapidly, and it is very rare for a physician to encounter this illness even in the developing world. Clinical findings can be easily overlooked in a busy OPD setting if the index of suspicion is low.




