Bieżący numer
Archiwum
Online first
O czasopiśmie
Redakcja
Rada Naukowa
Wydawca
Standardy etyczne i procedury
Bazy indeksacyjne
Recenzenci
Recenzenci Honorowi
Prenumerata
Kontakt
Najczęściej czytane artykuły
Dla autorów
Opłata za przetwarzanie artykułu (APC)
Książki i Konferencje
Książki
Konferencje
SARS CoV-2/COVID-19
PRACA ORYGINALNA
Diagnostic accuracy and clinical utility of the EARP questionnaire for detecting early psoriatic arthritis: a Turkish multicenter validation study
1
Department of Rheumatology, Denizli State Hospital, Denizli, Turkey
2
Department of Dermatology, Pamukkale University, Denizli, Turkey
Data nadesłania: 25-10-2025
Data ostatniej rewizji: 18-11-2025
Data akceptacji: 19-01-2026
Data publikacji online: 31-03-2026
Autor do korespondencji
SŁOWA KLUCZOWE
psoriatic arthritispsoriasisscreeningEARPvalidationdiagnostic accuracyearly detectionTurkish population
DZIEDZINY
STRESZCZENIE
Objectives:
Psoriatic arthritis (PsA) is a common but frequently underdiagnosed comorbidity of psoriasis, and early recognition is essential to prevent irreversible joint damage. The Early Arthritis for Psoriatic Patients (EARP) questionnaire is a brief and sensitive screening tool, yet a validated Turkish version has been lacking. This study aimed to linguistically adapt the EARP into Turkish, evaluate its psychometric properties, and determine its diagnostic accuracy for detecting PsA in dermatology practice.
Material and methods:
This multicenter cross-sectional diagnostic study included 119 adults with dermatologist-confirmed psoriasis. Psoriatic arthritis diagnosis was established according to Classification Criteria for Psoriatic Arthritis (CASPAR). The EARP was translated using standardized forward–backward procedures and pilot-tested for cultural relevance. Internal consistency (Cronbach’s a) and test–retest reliability (ICC2,1) were assessed. Diagnostic performance was analyzed through receiver operating characteristic (ROC) curves, yielding area under the curve (AUC), sensitivity, specificity, and predictive values at the optimal cut-off determined by Youden’s index.
Results:
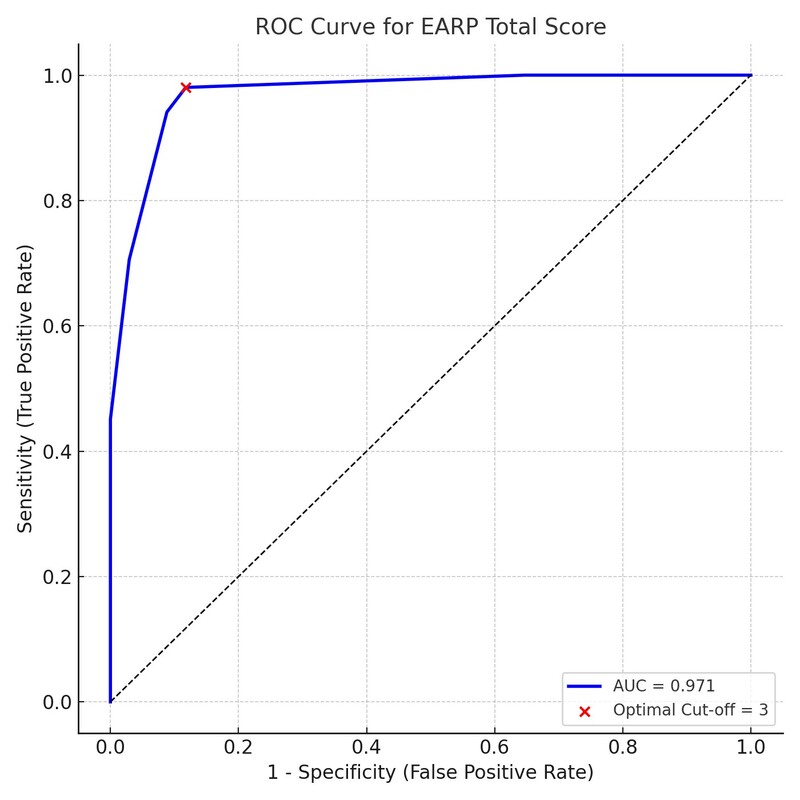
Psoriatic arthritis was diagnosed in 51 participants (42.9%). The Turkish EARP demonstrated high reliability, with Cronbach’s a = 0.86 and ICC2,1 = 0.998. Discriminative validity was strong: mean scores were significantly higher in PsA patients than in non-PsA individuals (6.47 ±1.99 vs. 1.74 ±1.35; p < 0.001). The ROC analysis showed excellent diagnostic accuracy (AUC = 0.971; 95% CI: 0.94–0.99). With the optimal cut-off ≥ 3, sensitivity reached 98.0%, specificity 88.2%, positive predictive value 86.2%, and negative predictive value 98.4%. Most false positives arose in individuals with fibromyalgia-like or mechanical pain symptoms.
Conclusions:
The Turkish EARP is a valid, reliable, and clinically practical instrument for early PsA screening in dermatology settings. Routine implementation may enhance diagnostic timeliness, reduce missed PsA cases, and support efficient referral to rheumatology.
Psoriatic arthritis (PsA) is a common but frequently underdiagnosed comorbidity of psoriasis, and early recognition is essential to prevent irreversible joint damage. The Early Arthritis for Psoriatic Patients (EARP) questionnaire is a brief and sensitive screening tool, yet a validated Turkish version has been lacking. This study aimed to linguistically adapt the EARP into Turkish, evaluate its psychometric properties, and determine its diagnostic accuracy for detecting PsA in dermatology practice.
Material and methods:
This multicenter cross-sectional diagnostic study included 119 adults with dermatologist-confirmed psoriasis. Psoriatic arthritis diagnosis was established according to Classification Criteria for Psoriatic Arthritis (CASPAR). The EARP was translated using standardized forward–backward procedures and pilot-tested for cultural relevance. Internal consistency (Cronbach’s a) and test–retest reliability (ICC2,1) were assessed. Diagnostic performance was analyzed through receiver operating characteristic (ROC) curves, yielding area under the curve (AUC), sensitivity, specificity, and predictive values at the optimal cut-off determined by Youden’s index.
Results:
Psoriatic arthritis was diagnosed in 51 participants (42.9%). The Turkish EARP demonstrated high reliability, with Cronbach’s a = 0.86 and ICC2,1 = 0.998. Discriminative validity was strong: mean scores were significantly higher in PsA patients than in non-PsA individuals (6.47 ±1.99 vs. 1.74 ±1.35; p < 0.001). The ROC analysis showed excellent diagnostic accuracy (AUC = 0.971; 95% CI: 0.94–0.99). With the optimal cut-off ≥ 3, sensitivity reached 98.0%, specificity 88.2%, positive predictive value 86.2%, and negative predictive value 98.4%. Most false positives arose in individuals with fibromyalgia-like or mechanical pain symptoms.
Conclusions:
The Turkish EARP is a valid, reliable, and clinically practical instrument for early PsA screening in dermatology settings. Routine implementation may enhance diagnostic timeliness, reduce missed PsA cases, and support efficient referral to rheumatology.
REFERENCJE (27)
1.
Ogdie A, Weiss P. The epidemiology of psoriatic arthritis. Rheum Dis Clin North Am 2015; 41: 545–568, DOI: 10.1016/j.rdc.2015.07.001.
2.
Azuaga AB, Ramírez J, Cañete JD. Psoriatic arthritis: pathogenesis and targeted therapies. Int J Mol Sci 2023; 24: 4901, DOI: 10.3390/ijms24054901.
3.
Coates LC, Helliwell PS. Psoriatic arthritis: state-of-the-art review. Clin Med (Lond) 2017; 17: 65–70, DOI: 10.7861/clinmedicine.17-1-65.
4.
Bagel J, Schwartzman S. Enthesitis and dactylitis in psoriatic disease: a guide for dermatologists. Am J Clin Dermatol 2018; 19: 839–852, DOI: 10.1007/s40257-018-0374-8.
5.
Haroon M, Gallagher P, FitzGerald O. Diagnostic delay of more than 6 months contributes to poor radiographic and functional outcome in psoriatic arthritis. Ann Rheum Dis 2015; 74: 1045–1050, DOI: 10.1136/annrheumdis-2013-204858.
6.
Alinaghi F, Calov M, Kristensen LE, et al. Prevalence of psoriatic arthritis in patients with psoriasis: a systematic review and meta-analysis. J Am Acad Dermatol 2019; 80: 251–265.e19, DOI: 10.1016/j.jaad.2018.06.027.
7.
Eder L, Polachek A, Rosen CF, et al. Development of psoriatic arthritis is preceded by nonspecific musculoskeletal symptoms: a prospective study. Arthritis Rheumatol 2017; 69: 622–629, DOI: 10.1002/art.39907.
8.
Lopez-Medina C, Kalyoncu U, Gossec L. Unmet needs in psoriatic arthritis: a narrative review. Arch Rheumatol 2024; 39: 159–171, DOI: 10.46497/ArchRheumatol.2024.10070.
9.
Tillett W, Jadon D, Shaddick G, et al. A systematic review of psoriatic arthritis screening tools. Ann Rheum Dis 2016; 75: 153–159, DOI: 10.1136/annrheumdis-2014-206971.
10.
Iragorri N, Hazlewood G, Manns B, et al. Psoriatic arthritis screening: systematic review and meta-analysis. Rheumatology (Oxford) 2019; 58: 692–707, DOI: 10.1093/rheumatology/key307.
11.
Tinazzi I, Adami S, Zanolin EM, et al. The Early Psoriatic Arthritis Screening Questionnaire (EARP). Rheumatology (Oxford) 2012; 51: 2058–2063, DOI: 10.1093/rheumatology/kes157.
12.
Lajevardi V, Ghodsi SZ, Shafiei M, et al. Evaluating Persian versions of EARP and PEST in Iranian psoriatic patients. Turk J Med Sci 2021; 51: 159–166, DOI: 10.3906/sag-2002-61.
13.
Alpsoy E, Emek M, Vardar C, et al. Psoriasis frequency in Antalya, Türkiye. Turk J Dermatol 2025; 19: 87–90, DOI: 10.4274/tdd.galenos.2025.39660.
14.
Kaymaz S, Karasu U, Kaçar N, Alkan H. Validity and reliability of the Turkish version of PEST. Arch Rheumatol 2022; 37: 483–494, DOI: 10.46497/ArchRheumatol.2022.8736.
15.
Duruöz MT, Şanal Toprak C, Ulutatar F. Validation of the Toronto Psoriatic Arthritis Screen II (ToPAS II) in Turkish patients. Rheumatol Int 2018; 38: 255–259, DOI: 10.1007/s00296-017-3844-3.
16.
Kaymaz S, Karasu U, Kaçar N, et al. Validation of the Simple Psoriatic Arthritis Screening (SiPAS) tool in Türkiye. Int J Rheum Dis 2020; 23: 1159–1164, DOI: 10.1111/1756-185X.13921.
17.
Choe YB, Park CJ, Yu DY, et al. Usefulness of PASE to monitor psoriasis: EPI-PSODE study. Ann Dermatol 2019; 31: 29–36, DOI: 10.5021/ad.2019.31.1.29.
18.
Mease PJ, Palmer JB, Hur P, et al. Utilization of validated PEST to identify PsA: Corrona Registry. J Eur Acad Dermatol Venereol 2019; 33: 886–892, DOI: 10.1111/jdv.15375.
19.
Oyur KB, Engin B, Hatemi G, et al. Turkish PASE: validation of PASE questionnaire. Ann Dermatol 2014; 26: 457–461, DOI: 10.5021/ad.2014.26.4.457.
20.
García-Gavín J, Pérez-Pérez L, Tinazzi I, et al. Spanish cultural adaptation of the EARP questionnaire. Actas Dermosifiliogr 2017; 108: 924–930, DOI: 10.1016/j.ad.2017.05.002.
21.
You HS, Kim GW, Cho HH, et al. Screening for PsA in Korean psoriasis patients using PASE. Ann Dermatol 2015; 27: 265–268, DOI: 10.5021/ad.2015.27.3.265.
22.
Haroon M, Gallagher P, FitzGerald O. Diagnostic delay and outcome in PsA. Ann Rheum Dis 2015; 74:1045–1050, DOI: 10.1136/annrheumdis-2013-204858.
23.
Karmacharya P, Wright K, Achenbach SJ, et al. Diagnostic delay in PsA: population-based study. J Rheumatol 2021; 48: 1410–1416, DOI: 10.3899/jrheum.200741.
24.
Gisondi P, Bellinato F, Galeone C, et al. Risk of PsA in psoriasis patients initiating biologics. Ann Rheum Dis 2025; 84: 435–441, DOI: 10.1136/ard-2024-225884.
25.
Rekha PR, Chandran V. Fibromyalgia in PsA: prevalence and impact. J Rheumatol 2021; 48: 1042–1048, DOI: 10.3899/jrheum.200613.
26.
Mease PJ, Etzel CJ, Helliwell PS, et al. Central sensitization in PsA and OA. Arthritis Care Res 2022; 74: 1339–1347, DOI: 10.1002/acr.24727.
27.
Shaddick G, Jadon D, Tillett W, et al. Machine learning-based prediction of PsA in psoriasis: PSORT consortium. Ann Rheum Dis 2023; 82: 1171–1179, DOI: 10.1136/ard-2023-224050.
Copyright: © Narodowy Instytut Geriatrii, Reumatologii i Rehabilitacji w Warszawie. This is an Open Access journal, all articles are distributed under the terms of the Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International (CC BY-NC-SA 4.0) License (https://creativecommons.org/licenses/by-nc-sa/4.0/), allowing third parties to copy and redistribute the material in any medium or format and to remix, transform, and build upon the material, provided the original work is properly cited and states its license.
Udostępnij
ARTYKUŁ POWIĄZANY
Przetwarzamy dane osobowe zbierane podczas odwiedzania serwisu. Realizacja funkcji pozyskiwania informacji o użytkownikach i ich zachowaniu odbywa się poprzez dobrowolnie wprowadzone w formularzach informacje oraz zapisywanie w urządzeniach końcowych plików cookies (tzw. ciasteczka). Dane, w tym pliki cookies, wykorzystywane są w celu realizacji usług, zapewnienia wygodnego korzystania ze strony oraz w celu monitorowania ruchu zgodnie z Polityką prywatności. Dane są także zbierane i przetwarzane przez narzędzie Google Analytics (więcej).
Możesz zmienić ustawienia cookies w swojej przeglądarce. Ograniczenie stosowania plików cookies w konfiguracji przeglądarki może wpłynąć na niektóre funkcjonalności dostępne na stronie.
Możesz zmienić ustawienia cookies w swojej przeglądarce. Ograniczenie stosowania plików cookies w konfiguracji przeglądarki może wpłynąć na niektóre funkcjonalności dostępne na stronie.